Healthcare Payer Payment Integrity Solutions PEAK Matrix™ Assessment 2020
Claims processing is becoming ever more complex for payers given issues such as the need to transform healthcare plans’ business models to accommodate new markets and new lines of business; and increasing inflow of members; and, increasing regulatory mandates. Payment integrity is a potential help – in can reduce rising healthcare waste and fraud to ensure that the medical claims are paid correctly and free of wasteful and abusive practices.
Payers’ traditional pay and chase approach has resulted in provider abrasion and has limited the recovery of over-/incorrectly paid claims. Payment integrity product vendors provide solutions that analyze a claim in both the pre- and post-submission phases, using advanced analytics and data mining tools and solutions. They use patterns identified across billions of lines of claims to predict errors, helping payers make required corrections before processing claims.
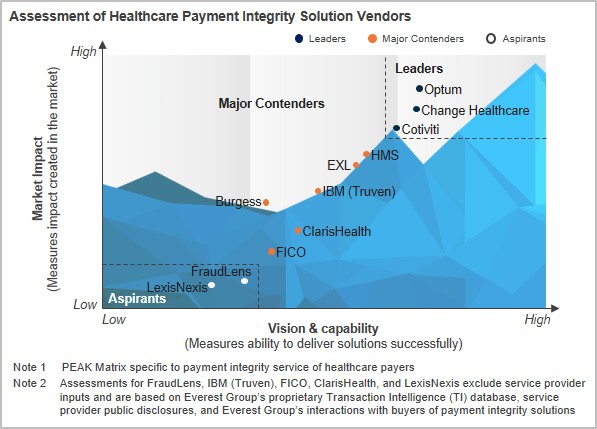
In this report, we analyze 11 payment integrity solutions vendors’ capabilities and map them on the Everest Group PEAK Matrix™, a composite index of distinct metrics related to a vendor’s vision & capability and market impact. This report offers:
- Market trends for payment integrity and the associated solutions market
- Information on the payment integrity solutions vendor landscape
- An assessment of the vendors on several vision & capability- and market impact-related dimensions
Vendors covered:Burgess, Change Healthcare, ClarisHealth, Cotiviti, EXL, FICO, FraudLens, HMS, IBM (Truven), LexisNexis, and Optum
Scope of this report:
- Industry: Healthcare payers
- Services: Payment integrity solutions
- Geography: US
Content:
This report has four key sections, each containing insights into the payment integrity solutions landscape:
- Summary of key messages
- Payment integrity solutions – market overview
- PEAK Matrix for payment integrity solutions, which maps vendors on the Everest Group PEAK Matrix and analyzes individual vendor capabilities along the following dimensions:
- Vision and capability
- Vision and strategy
- Technology capability
- Services capability
- Innovation and investments
- Engagement and commercial model
- Market impact
- Market adoption
- Portfolio mix
- Value delivered
- Profiles of payment integrity solution vendors:
- Vendor vision and strategy related to payment integrity solutions
- General overview of the vendor’s payment integrity solutions business – scale, overall focus, scope, and extent of adoption across enterprise lines of business, processes, and buyer sizes
- Overview of the vendor’s payment integrity solutions
- Assessment of the vendor’s payment integrity domain investments and innovative initiatives, and partnerships/alliances
